Bill expands access to overdose-reversing drug
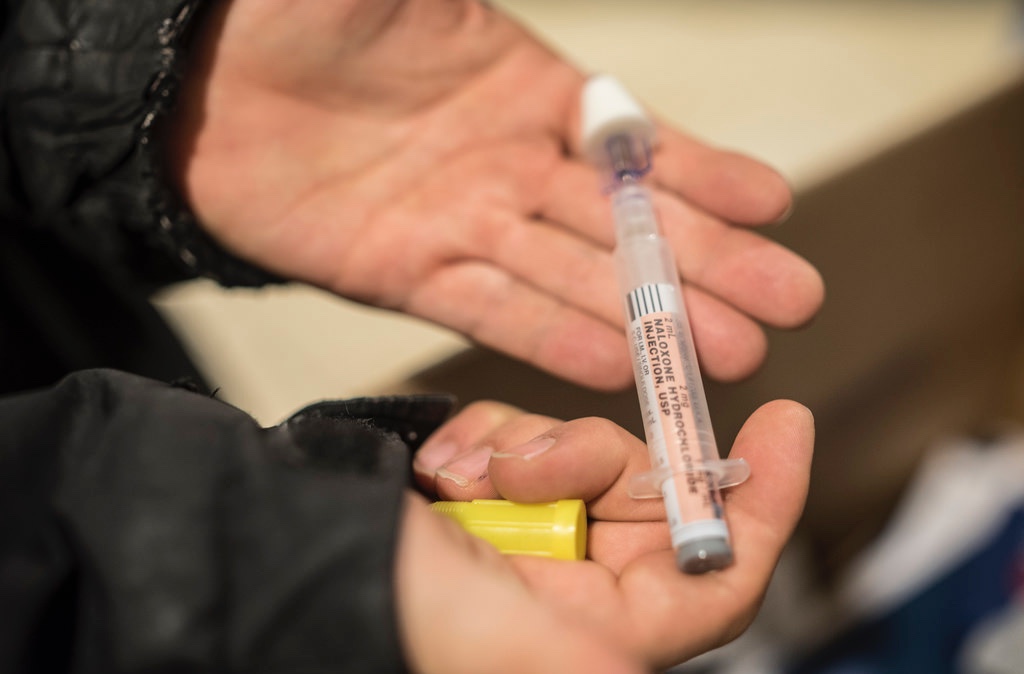
As opiate overdose deaths rise in Virginia, the General Assembly is moving to approve legislation intended to curb the epidemic. Three bills would expand access to naloxone, which reverses heroin and opiate overdoses and can be administered by friends and family of drug users.
By Craig Zirpolo
In a lecture hall at Virginia Commonwealth University, two presenters unpack a CPR mannequin as 30 students take their seats. While the scene resembles a first-aid class, trainers Rose Bono and Stephen Doheney are actually on the front line of a program combating the opiate overdose epidemic in Virginia.
After the two-hour course, the students will have qualified for civil immunity to administer naloxone, a life-saving drug that reverses heroin and opiate overdoses. As overdose deaths rise statewide, lawmakers in the House and Senate have advanced three bills that would expand access to naloxone across Virginia.
Del. Todd Gilbert, R-Woodstock, introduced HB 1833, which would expand naloxone access to law enforcement agencies. It unanimously cleared the House Courts of Justice Committee and is awaiting consideration by the full House.
HB 1458 and SB 1186 would give first responders and the general public more access to naloxone, provide civil protection to those who administer the drug, and allow family and friends of opiate users to obtain prescriptions. The House has passed HB 1458 and sent it to the Senate. The Senate Education and Health Committee unanimously endorsed SB 1186, which is now before the full Senate.
Heroin overdose deaths in Virginia more than doubled from 100 in 2011 to 213 in 2013, according to the Office of the Chief Medical Examiner. Every region of the state experienced an increase in heroin fatalities: They were up 164 percent in Northern Virginia, 94 percent in Hampton Roads and 50 percent in the Richmond metro area.
In September, Gov. Terry McAuliffe established the Governor’s Task Force on Prescription Drug and Heroin Abuse, which will recommend ways to reduce the stigma of overdose and addiction and promote access to naloxone. Naloxone is an “opioid antagonist” that reverses an overdose by blocking receptors in the brain before the victim stops breathing. Naloxone has been used in emergency rooms since the 1960s, but it has received attention for widespread use only recently.
Since 1996, more than 53,000 people nationwide have received training on administering naloxone, saving nearly 10,200 lives, according to the U.S. Centers for Disease Control and Prevention. In 2013, the Virginia General Assembly, led by Del. John O’Bannon, R-Henrico, began a pilot program called “REVIVE!”, headed by the Virginia Department of Behavioral Health and Developmental Sciences. The program is based on Project Lazarus, a similar initiative to curb overdose deaths in North Carolina. The Virginia program focuses on heroin in Richmond and prescription opiates in Southwest Virginia.
The program trained 187 people to lead naloxone administration sessions for members of the public. They in turn have trained 339 lay rescuers, including U.S. Sen. Tim Kaine. No trainer or lay rescuer has reversed an overdose with naloxone training obtained through the program yet.
A report on the pilot program said it faces obstacles such as the criminal stigmas of overdose and addiction and the difficulty of reaching active users. Cost also is a barrier: Naloxone can run $40-60 per dose with insurance and upwards of $300 without insurance. In addition, some pharmacies do not stock naloxone because demand can be relatively low.
Naloxone can be injected into a vein or muscle or administered as a nasal spray. The pilot program covers only nasal administration, so volunteers don’t have to use needles. Beyond its singular use in reversing overdoses, naloxone has no other effects on the body or potential for abuse, experts say. Because naloxone is safe and easy to administer, it is an ideal component of the grassroots campaign to help people at risk of an opiate overdose.
“It is hard to reach active users with top-down training,” said Rose Bono, who is pursuing a master’s of public health student at VCU. She led her first naloxone training session at the university in January. “We wanted to reach students because young people are at risk, but also because harm-reduction student organizations like Students for Sensible Drug Policy at VCU spread the information to other at-risk groups.”
Bono and Stephen Doheney worked with Karlotta van den Hurk, president of the campus chapter of Students for Sensible Drug Policy, to organize the training at VCU. “Beyond giving attendees the knowledge and confidence to properly handle overdose situations, I hope that events like this remind people in our community that using drugs doesn’t make a person’s life less valuable or worth protecting,” van den Hurk said.
Kyle Hughes attended the training at VCU and volunteers with DanceSafe, which focuses on the electronic music community. “Opiates are not the most prevalent substances at shows in my experience, but if I’m in the position to help prevent one overdose, the training is worth it,” Hughes said.
A final report on the pilot program recommended:
- Expanding statewide access to naloxone for law enforcement officers, other first responders and the public
- Increasing funding for naloxone kits
- Passing a medical amnesty law that would promote 911 calls by offering immunity to a person calling for medical help
Del. Betsy Carr, D-Richmond, proposed legislation to provide such immunity. HB 1500 would establish an “affirmative defense” for people who contact 911 to report an overdose emergency. Carr’s bill won a unanimous endorsement last week from the House Courts of Justice Committee and is now before the full House.
Bono said the bills before legislators this session could mean the difference between life and death. “If the General Assembly expands access to naloxone, there is a lot we can do to reduce the overdose epidemic in Virginia,” Bono said. “It is very rare to find a drug that has zero abuse potential and can immediately save lives.”
-
Recommend this
on Facebook -

Report an error
-

Subscribe to our
Weekly Digest



There is 1 reader comment. Read it.